
The Coronavirus pandemic has no doubt changed so much about the world we live in. It has also directly affected millions who either have or know people that have been diagnosed with this condition. As of Wednesday, June 10, it has claimed the lives of over 400,000 people.
Even though there appears to be a glimmer of hope with many states and countries opening back up in different ways over the past couple of days there are still many who are dealing with this horrible disease. That couldn’t be truer for gay couple Matt and Greg, the latter of which is still in recovery mode after being diagnosed with COVID-10 in mid-March.
What Greg has had to go through is truly heartbreaking according to his longtime partner who has been by his side to the best of his abilities over the past three months.
Matt was nice enough to talk with us at Instinct exclusively about the timeline of Greg’s diagnosis, the difficulties in having to mostly deal with this from a distance, his frank thoughts on people thinking that COVID is a hoax and so much more. Take a look.

When did your partner find out he had COVID?
Greg was tested on Wednesday, March 18, and received his positive result on Friday, March 20.
Did he experience any of the common symptoms prior to his diagnosis?
On the morning of Wednesday, March 18, 2020, he had gone into work at his clinic and felt a bit tired, but we were also returning home from a trip to Dallas the night before, so he assumed it was just fatigue. By lunch time, he had developed a headache and sore throat, and given the fact he is a physician (general practitioner/family doctor), he was sent home to isolate. Before leaving the office, he was swabbed by a colleague and brought home swabs for my best friend and me. During the two days that followed, he developed a fever, and he seemed to progress toward recovery for around a week, then he took a turn for the worse when he developed a very bad cough. He was admitted to the hospital and then immediately to the ICU on March 26.
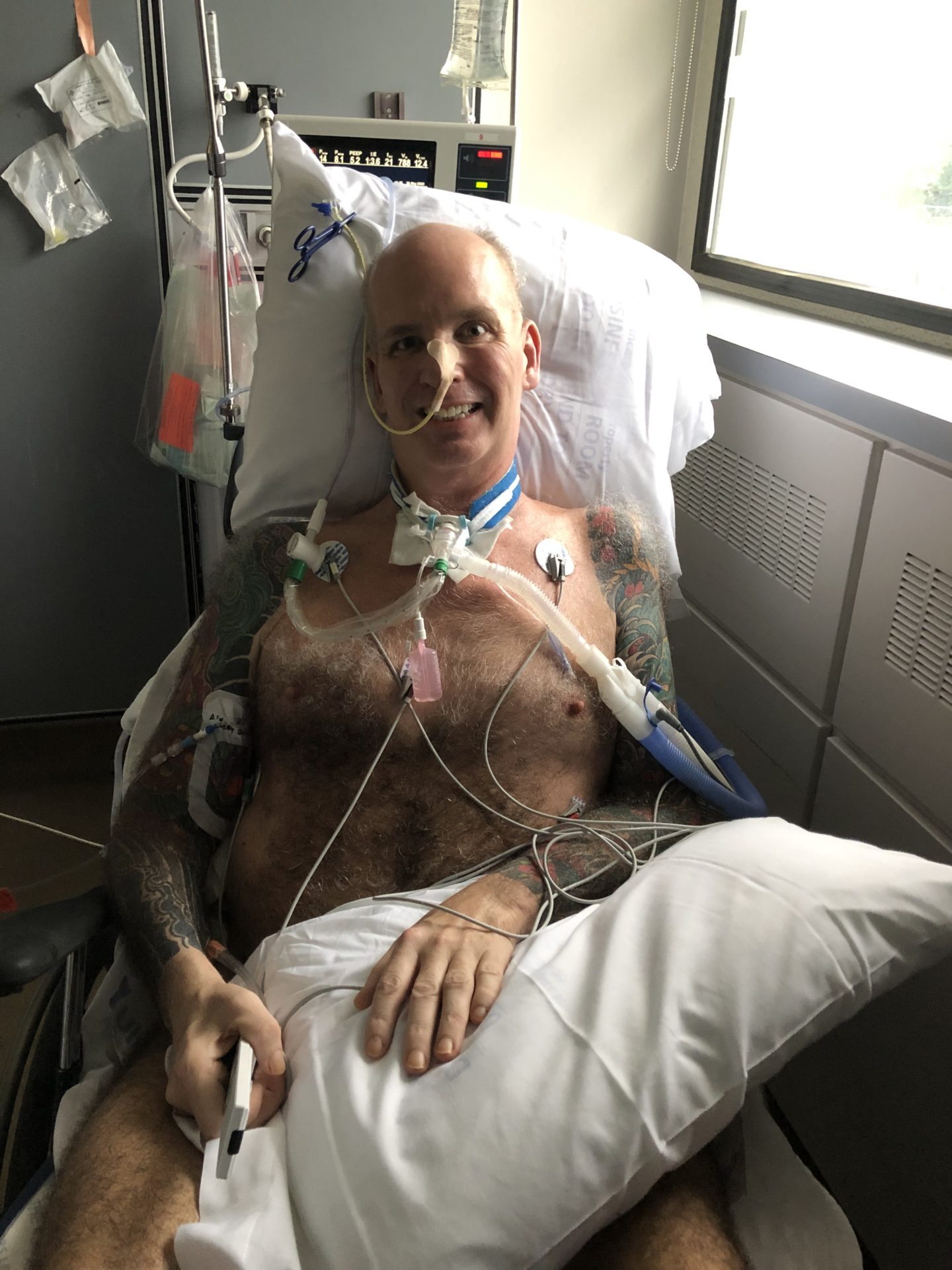
What has been the most difficult thing for you to endure as he battles this virus?
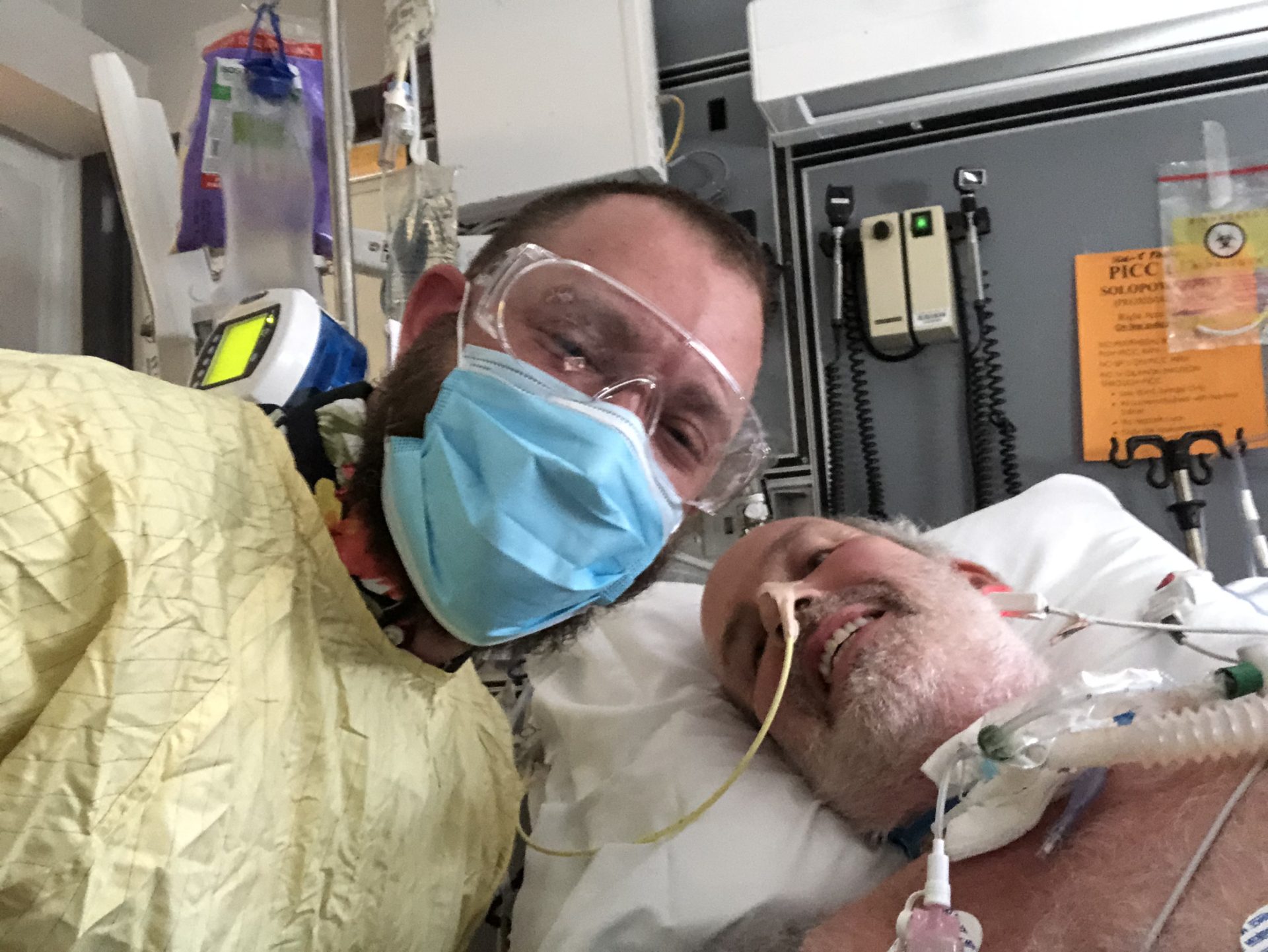
The biggest challenge has been the ban on visitors to the hospital (save for an exception that was made on day 54 of his stay in ICU where I was able to visit him for just over an hour). Since I am unable to visit, I have been limited to telephone updates from the nursing staff and physicians. The nursing staff can communicate his vitals and basic information about how Greg’s day has gone recovery wise, but it is the doctor who needs to communicate information regarding prognosis and treatment plans. Some of the doctors really stepped up during this crisis and were very timely with daily calls and very empathetic, while others could not be bothered to pick up the phone (in spite of being ordered to do so by the head of the ICU).
From approximately 11am until 3pm (the usual window I would receive an update from the various physicians overseeing Greg’s care), I would be a nervous wreck, completely paralyzed with fear. I couldn’t eat, I couldn’t even go to the bathroom for fear of missing the physician’s call and end up playing endless phone tag trying to figure out how Greg was doing. For the better part of 6-7 weeks, Greg was either in an induced coma, heavily sedated, delirious, or cognitively impaired because the virus was attacking his brain, so those calls were my lifeline. Once his condition improved and Greg was beginning to be able to communicate on his own, I was able to rest a bit more easily and started getting projects done while waiting for the doctor’s call.
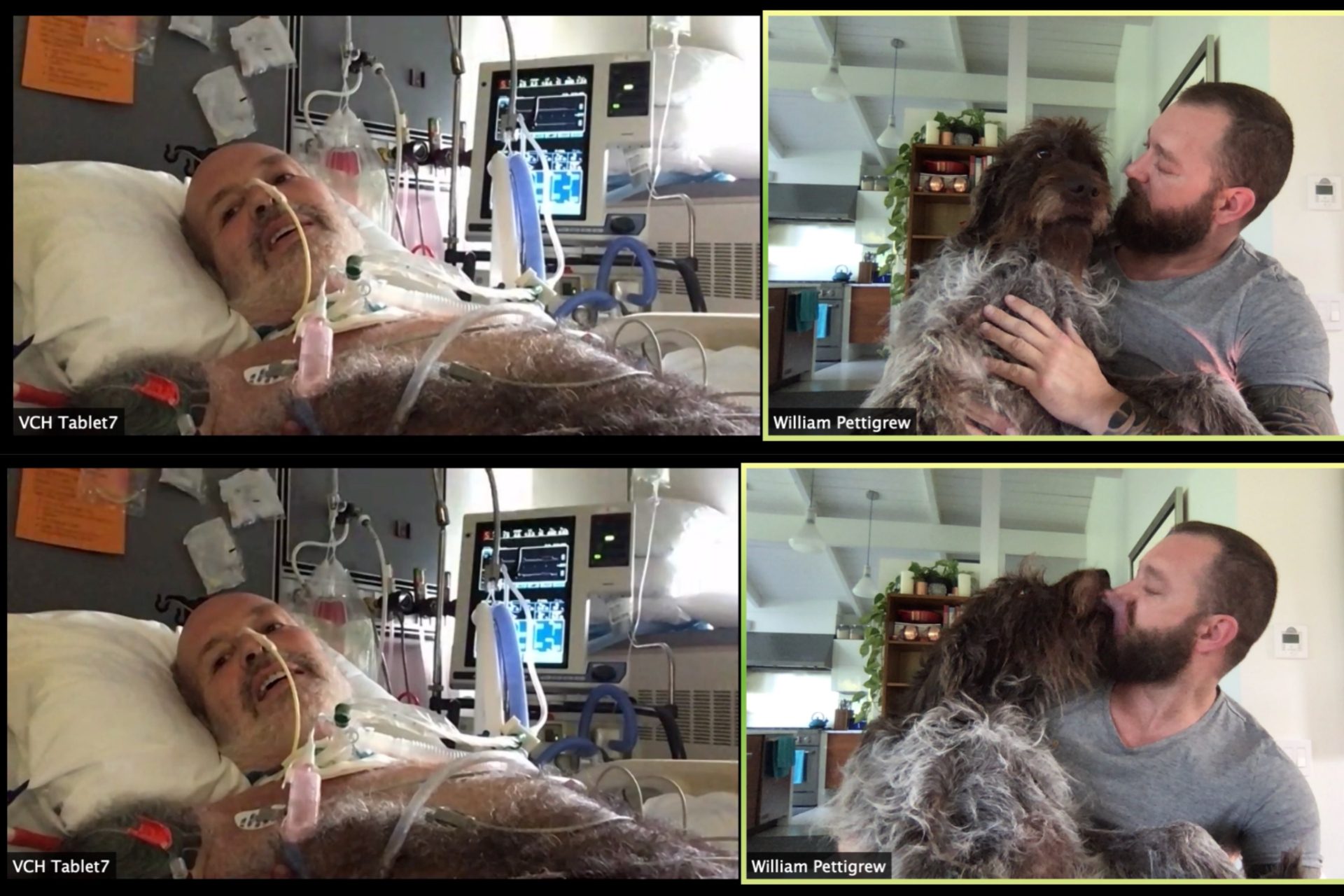
The only way of communicating with Greg regularly (once his cognition improved) was a daily Zoom Meeting at 6pm. Prior to that, they would point the video screen at him when he was either unconscious or semi-conscious and he might raise an eyebrow or smile with his eyes when he was awake, but sometimes those calls were harder than not seeing him at all.
How is he doing today and is he in recovery mode yet?
As of this morning, day 69 of his stay in the ICU, Greg is finally off the ventilator and was decannulated (tracheostomy removed). Within the next 24 hours he will likely be moved to a rehabilitation unit to work on physiotherapy and restrengthening. He went into the ICU at 6’6 and approximately 280-290 pounds (muscular, but with a bit of a belly) and he now weighs just over 200 pounds. He cannot yet sit up on his own, as he is quite weak, and he has developed a nerve condition in his neck shoulder that has severely weakened his left arm. Now that he is free of the ventilator, physiotherapy should be a lot easier and will be the big focus to get him out of the hospital.
What do you say to people who think that COVID is a hoax?
Frankly, “F**k you!”. I have tried to remain calm and engage people by sharing my experiences with this disease. The ones who have called it a hoax have called me opportunistic, and accused me of pushing politics by voicing concerns about ending lockdowns in the context of what my husband and our family have endured. Their selfish and heartless responses are in such great contrast to the love and support that we have received that I have zero time to coddle people who deny facts and dispute science. If someone cannot look at a healthy man, a physician who has devoted 36 years of his adult life to helping people, who has been ravaged by a virus and had his family put through hell, and muster up an ounce of empathy and see how serious this is, they can fuck all the way off.

Finally, what are you most hopeful for with his health and your future as a couple together?
There is a strong chance that Greg’s lung capacity will never return fully (because of COVID-19 and the necrotizing pneumonia he contracted), and the neuropathy he is experiencing in his shoulder/arm is liable to plague him for a very long time too. I remain hopeful that these will not have an overtly negative impact on him in the next 3-6 months, and that he can get back to normal activities before too long. I am also thankful that he does not remember anything before the 6-7 week mark, because those were dark days. It is quite common for people having endured long stays in the ICU to experience heavy depression and PTSD, and he certainly is dealing with the former at this point. These wounds will heal in time, especially as he regains his mobility and visitor restrictions no longer remain (or he returns home to me, whatever comes first).
As far as the future goes, there are some big changes coming. We have always been very focused on maintaining a healthy relationship after more than thirteen years together, but I think we will be even more focused and dedicated going forward. We will also be reexamining our wills, power of attorney, finances etc. because you never know when something like this could hit, and when it did, neither of us foresaw that one of us would be 10+ weeks in the hospital.
Early retirement is also likely in the books for Greg. He’s devoted more than 40 years to the study and practice of medicine (16 years as an emergency doctor, 20 years as a family doc), so it is time for him to focus more on himself. And I support him fully if that is what he decides to do.
I will be holding him a lot closer than ever, and I was a big cuddler to begin with. Absence makes the heart grow fonder, but successfully navigating a crisis can make the heart grow stronger– that’s where I see us today and in years to come.


Hi Matt, I was wondering if you could pass on a message I sent to Greg via Facebook. I used to work with Greg in Edmonton and I truly missed him when he moved on. From afar I have frequently prayed for him during this horrendous experience, and it is with relief, to finally see him smile as he heads on the road to recovery. Although this surely will be the darkest of times for both of you, I know both of you will forge forward together stronger than ever. God bless you both.
Nina
Thank God Greg is on the mend! Greg has been my Doctor for over 15 years as well as my son’s for the past 3 years and he has always been there when I needed his advice and care. He is a wonderful man and I wish him the best in his road to recovery!
Hi Matt I don’t have the pleasure of knowing you but, I want to thank you for letting us know how he is doing and all the care and love you have for him. I known Greg for over 20 years, he is the best doctor I ever had. Please keep taking care of yourself and him And God bless you both
I am so happy to hear Greg is doing so much better. Matt, your eloquent and heartfelt documentaries of Greg’s progress kept me hopeful that he’d pull through because I knew you were advocating for him. I want to send a big hug to both of you for making it through to the other side stronger in some ways, than you were before. Thank you for documenting this, now make your movie
Lori